Sexually transmitted infections (STIs) are the most common cause of sores in the reproductive organs, and this condition may lead to a Genital Ulcer (a sore in the reproductive organ). Continue reading to learn more about Genital ulcers.
What is Genital Ulcer?
An open sore on the genital region, including the vulva, perianal region, anus, or penis is referred to as a genital ulcer. Infectious pathogens are the most prevalent cause of genital ulcers. Women’s genitals are covered by the vulva, which is the outermost section. Sores in this region are called vulvar ulcers. Vulvar ulcers may be very painful or not at all uncomfortable.
Symptoms of Genital Ulcer
Vulvar ulcers may appear as pimples or a rash at first, but they may quickly become infected. Alternatively, the lesions may occur as a result of skin fractures that reveal underlying tissue.
Some of the symptoms of vulvar ulcers:
- Itchiness
- Release or leakage of liquids
- Urinating that is difficult or uncomfortable
- Suffering from any kind of discomfort
- Lymph nodes that have become engorged
- Fever
Causes of Genital Ulcer
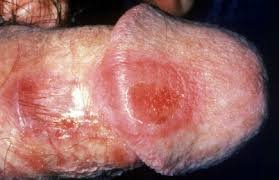
Photo credit: Wiley Online Library
A genital ulcer or a genital sore may be classified as either painful or non-painful depending on the kind of organism that is causing it (bacterial, virus, fungus, protozoa, and parasites). For simplicity, the ulcer or sore can be classified as either painful or non-painful.
The following are the causes of Genital Ulcers;
1. Genital Herpes
A virus is responsible for genital herpes. Small, painful blisters filled with a clear or straw-colored fluid might be characterized as the sore; lymphadenopathy occurs during the initial illness.
2. Reactions to drugs
NSAIDs, sulfonamides, and certain antibiotics may provoke an ulcer-inducing response in the body’s gastrointestinal tract.
3. Chancroid
Perineal lesions are prevalent in women or men who have had intercourse with males; painful inguinal lymphadenitis is a typical complication of this.
4. Syphilis
Painless inguinal lymphadenopathy in the early stages of infection; small, open sore or ulcer on the genitals (known medically as a “chancre”).
5. Pubic Lice
Blueish-gray bluish-gray macules (Pthirus pubis) that appear after being bitten by a pubic lice/crab (Pthirus pubis). It also causes severe itching.
6. Cancer
Ulcers surrounding the vagina might be a symptom of vulvar cancer. As women become older, they’re more likely to get this sort of cancer.
7. Lymphoma Venereum (LGV)
Lymphoma Venereum (LGV) is a bacterium. Symptoms of LGV include sensitive inguinal lymphadenopathy and a tiny, shallow, painless genital or rectal lump or ulcer.
8. Infection
The most frequent symptom of a yeast infection, or candidiasis, is a swollen, red, and itchy vulva with visible scratch marks.
9. Trichomoniasis
Trichomoniasis may produce labial ulcerations, cervical erosion, and many, minute punctate hemorrhages, as well as enlarged papillae on the cervix, in addition to the stinky fishy vaginal discharge.
10. Genital warts
They are also caused by a virus. Either elevated or flat and like the cauliflower’s head, ulcers are commonly spread sexually and often co-exist with other STDs.
11. Infections due to bacteria
Sores on the vulva may be caused by bacterial infections such as Group A Streptococcus and mycoplasma. Antibiotics are often used to treat bacterial infections.
12. Scabies
Sarcoptes scabiei hominis, a parasite that causes scabies, causes threadlike burrows with vesicules and papules on the genitals because it is very irritating to the touch.
13. Donovanosis
Donovanosis also known as granuloma inguinale, is a bacterially-caused STD. vaginal, groin, or perineal ulcers that are red and meaty in appearance but do not cause any discomfort or discomfort at all.
14. Skin repercussions
A vaginal ulcer might be caused by a poor response to skincare products. If this occurs, you may wish to use soaps and lotions designed for people with sensitive skin instead.
Other possible causes of genital ulcers
There are many other causes of genital sores outside sexually transmitted diseases, including rashes such as psoriasis, molluscum contagiosum, and allergic responses, as well as non-sexually transmitted viruses including Epstein-Barr virus and cytomegalovirus.
What are the side effects of a Genital Ulcer?
If you ignore a genital ulcer, it might lead to other health issues. Many health issues might result from vulvar ulcers that aren’t addressed.
- Sexually Transmitted Diseases
- Infections
- Scarring
- Inflammation
- Adhesions
When ulcers are caused by an underlying ailment, you may also suffer from additional issues as a result of this. Getting pregnant, for example, might be problematic if you have an STD. Syphilis, for example, has the potential to cause long-term complications including nerve damage and heart disease.
Treatment of Genital Ulcer
What’s causing your ulcers will dictate your treatment plan. Some genital ulcers may heal on their own, but in order to prevent infection, it is necessary to treat them right soon.
If you have a medical issue, your doctor may offer a variety of treatments to address it. Antibiotic and antiviral medications, either taken orally or intravenously, are often used to treat STIs.
The following are possible treatments for the genital ulcer that are not caused by an infection:
- methotrexate and other immunomodulatory medications
- corticosteroids
- antihistamines
Until it heals, ask your doctor or other health care professional for instructions on how to properly treat your ulcer. Additionally, you may need specialized dressings to keep the wound clean and safe.
Sometimes, genital sores may be alleviated with the use of home remedies. Among the most often used approaches are:
- The use of lidocaine or other topical anesthetics
- Wearing loose-fitting clothes and avoiding any products that may irritate your skin
- Taking a bath with Epsom salts
- Acetaminophen and other over-the-counter analgesics (Tylenol)
- Applying ice packs to the region where the injury occurred
- petroleum and zinc oxide-based barrier ointments